About pterygium
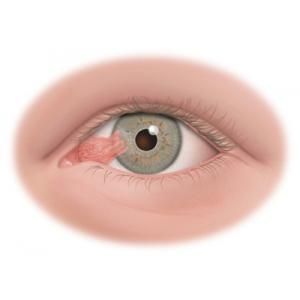
A pterygium is a benign triangular fibrovascular tissue that grows on the eye’s conjunctiva and can spread to the cornea limbus and beyond. The conjunctiva is the transparent membrane that lines the inside of the eyelids and covers the sclera (the white part of the eye).
Typically, a pterygium appears nasally. In its early stages it appears slightly red and as it progresses it may also contain vessels.
Factors leading to pathogenesis
- Ultraviolet Light (UV)
- Dry Environment
- Outdoor activities such as surfing or working in a field seem to be related with pterygium growth and that is why it is also called “surfer’s eye” or “farmer’s eye”
Pterygium may progress slowly and gradually cease to advance. Other times it progresses faster, covering the cornea and causing visual symptoms as it moves towards the pupil. In such advanced cases, treatment is recommended.
Symptoms
Early pterygium is usually asymptomatic and does not cause visual symptoms. As it grows, the ocular surface gets irritated and the patient may experience discomfort and a foreign body sensation.
In more advanced cases, the pterygium increases in size, invades the cornea and moves towards the pupil causing astigmatism. In severe cases, it may encroach onto the visual axis causing blurry vision
Evaluation & Diagnosis
For a proper evaluation, the following exams are necessary:
- Visual Acuity (VA) performance (with and without correction)
- Slit Lamp (S/L) (biomicroscopic evaluation of the eye and eyelids by the ophthalmologist)
- Keratometry (A/R) (cornea’s curvature)
- Cornea Tomography (Pentacam) (cornea’s curvature and pachymetry in various locations)
- Optical Coherence Tomography OCT (measures the cornea’s pachymetry in a 9mm wide area, as well as the outermost corneal layer, the epithelium, which is directly affected by the pterygium)
The diagnosis of pterygium is based on the clinical appearance of the lesion. Typical findings include:
- Fibrovascular conjunctival growth within the palpebral fissure extending onto the corneal surface
- Triangular shaped tissue extending onto the cornea
- Vascular straightening in the direction of the advancing head of the pterygium on the corneal surface
- May be a thin translucent membrane or significantly thickened with an elevated mound of gelatinous material
- It may affect the nasal and temporal limbus of both eyes or only a single location
- Raised lesion, white to pink in color depending on vascularity
- Ranges from a fine transparent area with very mild elevation, few vessels, and minimal corneal involvement in the early stages to a thick opaque vascular growth extending to the visual axis in later stages
- Pinguecula are often present in the ipsilateral or contralateral eye
- A pigmented epithelial iron line (Stocker’s line) adjacent to a pterygium is evidence of chronicity
It is unusual for pterygia to deviate from the characteristic locations of three and nine o’clock within the palpebral fissure. Pterygioid lesions in other locations should elevate suspicion for alternate diagnoses.
In any case, your eye doctor will explain how often he should monitor the size and texture of your pterygium.
Pterygium Management
Management varies depending on the pterygium’s location and severity.
In the early stages, lubricants such as ointments and artificial tears alongside mild anti-inflammatories can aid with symptoms such as irritation, redness and foreign body sensation.
In more advanced stages there is the option to surgically treat pterygium, either for cosmetic reasons or due to reduced vision.
During excision, the head and the body of the pterygium are removed and to prevent recurrence, we use adjunctive therapies such as subconjunctival corticosteroid injection and mitomycin.
There are two more techniques that can be used after the excision of the pterygium:
- A conjunctival autograft technique, which involves obtaining an autograft (conjunctiva) from another place on the surface of the eye and suturing the graft over the exposed scleral bed after excision of the pterygium.
- Amniotic membrane grafting, which is a tissue bandage placed over the bare sclera. The amniotic membrane promotes healing and reduces rates of recurrence. Usually, a large diameter bandage contact lens is inserted to keep the amnio in place. The amniotic membrane is being slowly absorbed within a few weeks.
Treatment Outcomes
In any of the above pterygium management options, the aesthetic result is satisfactory. The pterygium’s management becomes more complicated the more it extends towards the cornea.
Opacities on the cornea may be noted following pterygium removal and some may remain. The epithelium is also under stress after surgical pterygium removal, regardless of its natural regeneration, but the pterygium tissue removal is imperative, as it will restore the visual functions of the eye.
Individuals under 40 years old may have a pterygium recurrence, even having it surgically removed. To avoid its reappearance, one should avoid the environmental conditions that seem to cause the pterygium formation in the first place:
- Protection against UV light (using sunglasses, hats etc)
- Avoid exposure to environmental irritants eg: smoke, dust, wind and chemical pollutants
- Use of artificial lubricants (tears and ointments) in dry conditions


